Almost as thin as a sheet of paper, yet essential for seeing the world. It’s there corneathe outermost part of our eye. When this tissue becomes diseased or suffers serious damage, vision can become blurred, distorted, and even lost. Often, the only solution is a transplant. But what happens from the moment a person decides to donate their corneas to when they are shown again to another human being?
We entered the beating heart of these techniques, visiting the Banca degli Occhi Foundation in Mestre, one of the 12 banks that manage this delicate passage. Here is the story of an incredible journey, between advanced biology, micro-surgery and profound humanity.
What is the cornea and how is it made
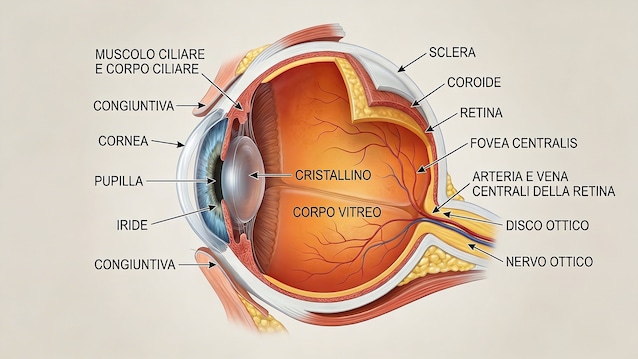
The cornea is the transparent membrane located in the most anterior part of the eye. It’s a very powerful lens. Its function is to capture light and direct it precisely towards the lens and then onto the retina, to then be transformed into electrical impulses that are processed by the brain.
It is a one-of-a-kind fabric: it has no blood vessels. It is nourished by oxygen in the air and nutrients present in the internal fluid of the eye. This absence of vessels is the secret of its perfect transparency. Although it is very thin (about half a millimeter in total), it is made up of several specialized layers:
- Epithelium: the outermost, protective layer.
- Stroma: the thickest part, made of collagen and “lazy” cells (keratocytes) that are activated only to repair damage.
- Endothelium: an inner layer of crucial cells that pump water out of the cornea to keep it transparent. Curiosity: these cells they do not regenerate. If they decrease too much, the cornea becomes opaque.
Due to its very high density of nerve endings, the cornea is one of the most sensitive tissues in the body. For this reason, some corneal pathologies cause intense and penetrating pain.
When the world becomes fog: corneal pathologies
When the cornea becomes damaged or diseased, vision is drastically affected. Patients do not necessarily live in total darkness, but in a state of low vision which invalidates daily life.
- Keratoconus: the cornea loses its spherical shape and becomes conical. Patients describe vision as distorted, “as if looking through a glass,” with elongated images. It often affects young people between 20 and 40 years old.
- Clouding and Infections: Severe infections (sometimes due to incorrect contact lens wear) or trauma can make the cornea cloudy. It’s like living in a perpetual fog.
For this type of pathology, the only solution may be a cornea transplant.
Inside the Eye Bank: a high-tech vault
The journey of the donated cornea begins immediately after the collection carried out by specialized doctors. The tissue is transported to one of the 12 Eye Banks present in Italy. The one in Mestre that we visited is an Italian excellence, a highly sophisticated laboratory that acts as a “bridge place” between donor and recipient.
Safety and Sterility
To enter the laboratory, the procedures are very strict. The standards are decided by the European Eye Bank Association.
The laboratory is an isolated environment, where the air pressure is kept higher compared to the outside to prevent the entry of dust and contaminants. You pass through a system of double interlocked doors. The staff wears special low particle release suits, headphones and double shoes. Even if the environment is ultra-protected, the corneas never touch the laboratory air: they are handled exclusively inside sterile cabins laminar flow.
Phase 1: Evaluation and Artificial Intelligence
As soon as it arrives, the cornea is identified and traced. The screening begins. The operator uses sophisticated tools such as slit lamp (the same one used by ophthalmologists) and the specular microscope . The fundamental parameter is the cell density of the endothelium. You need to count how many healthy cells are present per square millimeter. Today, this counting is supported by software equipped with Artificial intelligencewhich make the analysis very rapid and precise, even if the final validation always falls to the expert eye of the biologist.
Phase 2: Conservation
If suitable, the cornea is placed in a sterile bottle containing nutrient solutions and antibiotics. It is then stored in a incubator at 31°Cthe normal temperature of our eye. Here it can stay up to 30 days. Alternatively, it can be stored in the refrigerator at 4°C for two weeks.
This period is crucial not only for logistics, but for execution microbiological controls thorough tests that exclude bacteria, fungi or other pathogens. An interesting fact that has emerged in recent years: laboratories are experiencing an increase in contamination by yeasts and fungi, an indirect effect of global warming which influences the environmental microbial flora, and which tissue conservation must take into account.
Phase 3: “tailored” preparation and selective surgery
In the last twenty years, corneal surgery has made great strides, moving from “full thickness” transplantation (penetrating keratoplasty) to selective lamellar surgery. Today, often only the diseased layer is transplanted.
This is where the Eye Bank becomes an “antechamber to the operating room.” Hospitals submit specific requests via a digital portal. The Bank, like a high-precision tailor, prepares the fabric to measure.
Phase 4: Micrometric cutting
Using a very high precision instrument and checking the thickness with an examination OCT (Optical Coherence Tomography), the operator performs the cut. Thick corneal flaps can be obtained 200, 90 or even 20 microns (2 hundredths of a millimeter). We are talking about thicknesses similar to cling film.
Working such thin fabrics is very difficult. There is a risk of them rolling up or getting damaged. To help the surgeon in the operating room, the bank prepares the isolated tissue and marks it (for example with a letter) to indicate the correct direction for insertion into the eye. Finally, the tissue is placed in special sterile micro-containers.
Phase 5: the final act in the Operating Room
Once ready and sealed, the cornea travels via specialized couriers (or planes for very urgent cases) to one of over 200 transplant centers.
The “four-handed magic” takes place in the operating room, the result of collaboration between the biologist who prepared the tissue and the surgeon. The surgeon, after removing the diseased layer from the patient, inserts the very thin donated flap inside the eye. To adhere it to the recipient’s cornea, use a small air bubble, which will open the tissue and allow it to adhere to the eye. A quick gesture, with extreme precision, which allows the patient to see again often just a few hours after the operation.
Italy as Excellence and the Importance of the Gift
In Italy, thanks to the network coordinated by the National Transplant Center, approximately 8,400 corneal transplants per year. Our banks are an excellence that supplies fabrics not only nationally, but also abroad, especially where donation is less widespread or where technologically advanced preparations are needed.
However, the global need is immense. Compared to 185,000 transplants per year in the world, there are more 12 million people pending. Corneal diseases are the fifth cause of blindness worldwide.
Being able to see again means autonomy, being able to watch your children grow up, work, walk down the street without fear. Even those with vision defects such as myopia can be a donor.
Saying “yes” to organ and tissue donation, for example to renewing an identity card, is a simple gesture that can radically change a person’s vision and therefore their life.
