What really happens when an organ leaves a donor’s body to save another? It’s a race against time involving surgery, biology and complex logistics. In this in-depth study we take you “behind the scenes” of the operating room to understand how doctors challenge cell death through thermal shock and the perfusionfundamental techniques to keep the heart, liver and kidneys alive during transport, as explained by the National Transplant Center. We will analyze the numbers for 2024, a crucial year for Italian healthcare with beyond 4,600 transplantsbut also marked by a worrying increase in opposition, often based on unfounded fears. We will explain the rigorous award criteria of National Transplant Network and we will guide you through the ways to consciously express your choice. Because with over 8,000 people on the waiting list, understanding how the system works is the first step to trusting and saving lives.
We thank the Doctor De Panfilis of the resuscitation department of the Policlinico Umberto I of Rome and the National Transplant Center for technical support.
Organ harvesting and preservation
Let’s get straight to the point. We are in the operating room and it’s time for the blood sample. The donor’s body is treated with the utmost respect: the surgical techniques are the same as standard interventions and, at the end of the operation, the body is carefully recomposed, without leaving obvious aesthetic alterations.
However, there is an immediate biological challenge. At the exact moment in which the organ is detached from the blood circulation, the oxygen supply is eliminated. If the organ remained at body temperature of 37°Cthe cells would consume the last reserves of energy and the organ would “die” in a few minutes. Two fundamental procedures are activated. The thermal shock in which the organs are immediately “perfused”, i.e. passed through by a very cold solution (approx 4°C). This sudden cold drastically slows cellular metabolism, putting the organ into a sort of “pause mode” (standby). They are subsequently stored in sterile bags with ice.
In more complex cases, the dynamic perfusion: they are used sophisticated machinery which simulate blood circulation, pumping a liquid rich in oxygen and nutrients. This allows the cells to remain active, eliminate waste and arrive at the transplant in optimal conditions
At this point the stopwatch starts. Each organ has a maximum “ischemia time”, that is, a time limit for life outside the body:
- Heart and lungs: 3–5 hours
- Liver: 5–7 hours
- Kidneys: up to 12–18 hours
Before the withdrawal, the clinical evaluation of the organs that can be donatedwhich are heart, lungs, liver, kidneys, pancreas, intestine, corneas and tissues.
How to assign an organ
While the surgeons operate, the National Transplant Network he’s already at work. There are no preferential lanes or recommendations: the assignment takes place via a algorithm which cross-references the donor’s data with that of the patients on the waiting list. The criteria are rigorous and objective:
- Blood type;
- Immunological compatibility;
- Clinical urgency (those who risk their lives have priority);
- Time on waiting list;
- Organ size (physical compatibility).
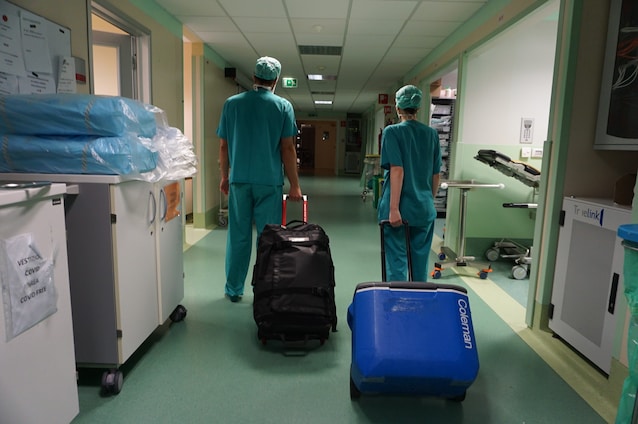
Once the recipient is identified, the organ sets off approved refrigerated cases. If the distance is short, road vehicles are used (ambulances, medical vehicles), but if time is short or the distance is long, we fly with planes.
From arrival at the hospital to the transplant
When the briefcase arrives at its destination, you don’t immediately rush to the operating room. There is one last step: final quality check. The team of surgeons checks the temperature, the integrity of the sacs and performs rapid tests on the organ. Only if everything is perfect can we proceed. At this point anesthetists, surgeons and nurses work in sync.
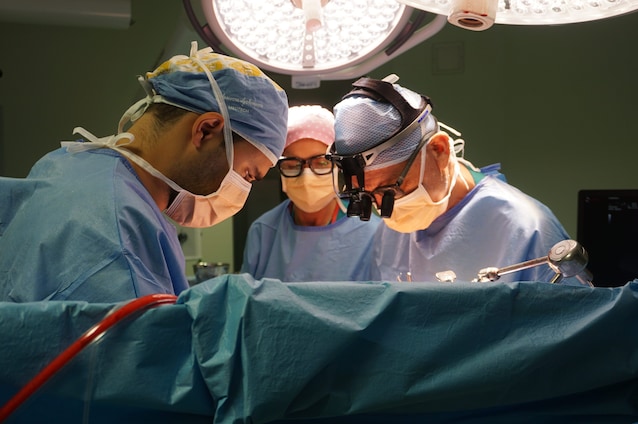
Those who work in this field assure that the moment in which the new organ is connected to the blood vessels, receives blood, regains color and starts functioning again, is one of the strongest emotions one can experience in medicine. From that moment, the patient will begin a immunosuppressive therapy (to avoid rejection), but will have a new lease on life.
4,642 transplants carried out in Italy in 2024: the data
Italy has an excellent transplant network. 2024 was a crucial year with 4,642 transplants carried out thanks to the donations of 1,730 donors. They were involved in this process 292 hospitals that have reported a potential donor e 42 hospitals equipped with dedicated transplantology teams.
The most transplanted organs in Italy are:
- Kidney: 74%
- Liver: 12%
- Heart: 9%
- Lung: 3%
- Pancreas: 2%
- Intestine: 0.1%
The kidney dominates the ranking for three reasons: chronic kidney diseases are very widespread, transplantation is a much more effective solution than dialysis and, unlike other organs, it can also be donated by a living person.
How to become a donor (and why to do it)
There is a fear that, unfortunately, stops many people: “If they know that I am a donor, will the doctors let me die to take my organs?”. The answer is a No categorically, legally and ethically, treatments cannot be influenced by donor status.
The path is divided into stagnant phases, managed by different teams who often don’t even know each other. THE’treatment team aims to save the patient’s life,death verification is performed by a third party commission and the withdrawal it occurs only when death is certified and irreversible. This is where transplant coordination comes in and you consult the SIT (Transplant Information System). If the citizen said YES, we proceed. If he said NO, we stop. If he has not expressed himself, the decision lies with the family (who in a moment of grief may not know the wishes of the deceased loved one).
Today in Italy there are more than 8,000 people on the waiting list. For a kidney, the average wait is approx 3 years. Unfortunately, opposition is on the rise: in 2025, the 41% of people said “NO” to renewing their identity card (an increase compared to 36.3% in 2024). The very young (18-30 years old) and the over 60s are most likely to say “no”. The rate of those who abstained (therefore did not choose) was 42% in 2024.
Certainly in the percentages of those who said no or did not express themselves there are many doubts about how the donation works and what are the ways to declare one’s choice.
In Italy every adult citizen can – without any obligation – express their will. NoThere is no age limit for donatingthe biological health of the organ counts, not the registry. The choice can be communicated in 4 ways:
- Al Commonupon renewal of the Identity Card (the most common method).
- On the website ofAIDO (aido.it) via SPID (immediate and online).
- AtASL reference by signing a form.
- With one written statement (card or sheet) to keep in your wallet.
The latest statement issued in chronological order always applies. Choosing today means removing a burden from your family members tomorrow and, above all, giving a chance in life to those who are waiting for that phone call that changes everything.